Men's Pelvic Health Physiotherapy in Sydney
Tom is one of Sydney's few male physiotherapists with dedicated specialist training in male pelvic health. At Atlas Physiotherapy in Leichhardt, he provides clear, respectful care for a wide range of men's pelvic health conditions - in an environment where these conversations feel normal, supported, and without judgement.

Reasons why people see us
Pelvic Floor Dysfunction
Pelvic floor physiotherapy for men in Sydney - treating weakness, tension, and poor coordination.
The Pelvic Floor Muscles
The pelvic floor is a group of muscles that sit at the base of the pelvis, stretching from the pubic bone at the front to the tailbone at the back. Think of them as a supportive, muscular bowl moving up and down as they contract and relax.
In men, these muscles:
Support the bladder and bowel
Help control urine and wind
Contribute to erectile rigidity
Assist with ejaculatory control
Support pressure management during lifting, coughing, and exercise
They work automatically most of the time, but they also need to contract and relax at the right moments. Like any muscle group, they can become weak, poorly coordinated, or overly tight.

Signs and Symptoms of Pelvic Floor Dysfunction
Pelvic floor issues are not just about weakness - dysfunction can also involve tension, overactivity, or poor coordination.
Possible symptoms include:
Urinary leakage (with cough, exercise, or urgency)
Difficulty fully emptying the bladder
Urinary frequency or urgency
Post-urination dribbling
Erectile instability
Premature ejaculation
Pelvic, perineal, or testicular pain
Pain with sitting
Constipation or straining
A feeling of pelvic heaviness or pressure
Many of these symptoms are common, but they are not something you simply have to live with.
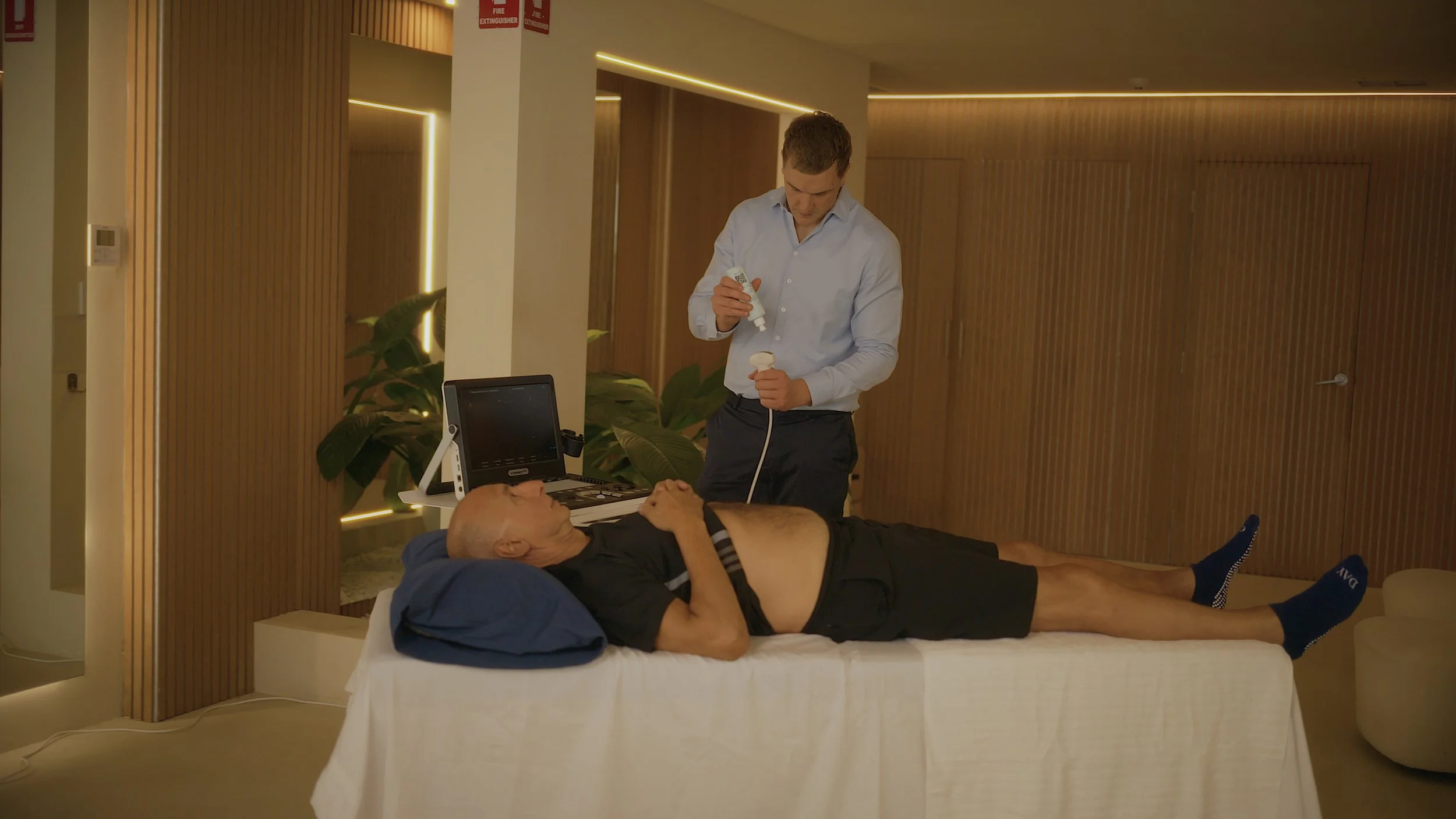
How Atlas Physiotherapy Can Help
Pelvic health physiotherapy focuses on restoring strength, control, and relaxation where needed.
Assessment may include:
Evaluating pelvic floor strength and endurance
Assessing coordination and timing
Identifying overactivity or muscle tension
Reviewing bladder, bowel, and sexual function
Assessing breathing and abdominal pressure patterns
Treatment may involve:
Targeted strengthening programs
Down-training and relaxation techniques
Bladder and bowel habit retraining
Breathing and pressure management strategies
Return-to-exercise planning
Education to build confidence and understanding
Pelvic floor rehabilitation is specific, structured, and tailored - not just “do your Kegels.”

Bladder Health Physiotherapy for Men - Sydney
Bladder symptoms affect a large proportion of men, particularly as they age or following prostate treatment. At Atlas Physiotherapy in Leichhardt, we assess the underlying causes of bladder dysfunction and create a targeted treatment plan - not just a list of exercises.
Normal Bladder Function
A healthy bladder is designed to store 300-400ml of urine comfortably and empty fully when you go to the bathroom. Most men will go 4-7 times a day, sleep through the night or wake once to urinate, and have good control over starting and stopping the flow.
Common bladder symptoms and problems
Bladder issues can develop when control or capacity is disrupted, possibly (but not always) due to changes of your prostate.
Symptoms may include:
Needing to get to the toilet in a hurry
Going more often
Getting up multiple times at night
Difficulty starting or maintaining the stream
Not being able to fully empty the bladder
Dribbling after you’ve finished
Not being able to hold it in
While common, these symptoms are not something men simply have to “put up with.”
How Atlas Physiotherapy Can Help
We understand these symptoms can be embarrassing and have a huge effect on confidence and your overall wellbeing.
At Atlas Physiotherapy we focus on understanding why bladder symptoms are occurring and how they fit with your overall health and lifestyle. Treatment may involve pelvic floor muscle retraining (strengthening or down-training), bladder retraining strategies to improve bladder storage, education around fluid and toileting habits.
The goal is to improve bladder control, confidence, and quality of life using practical, evidence-based strategies tailored to you.
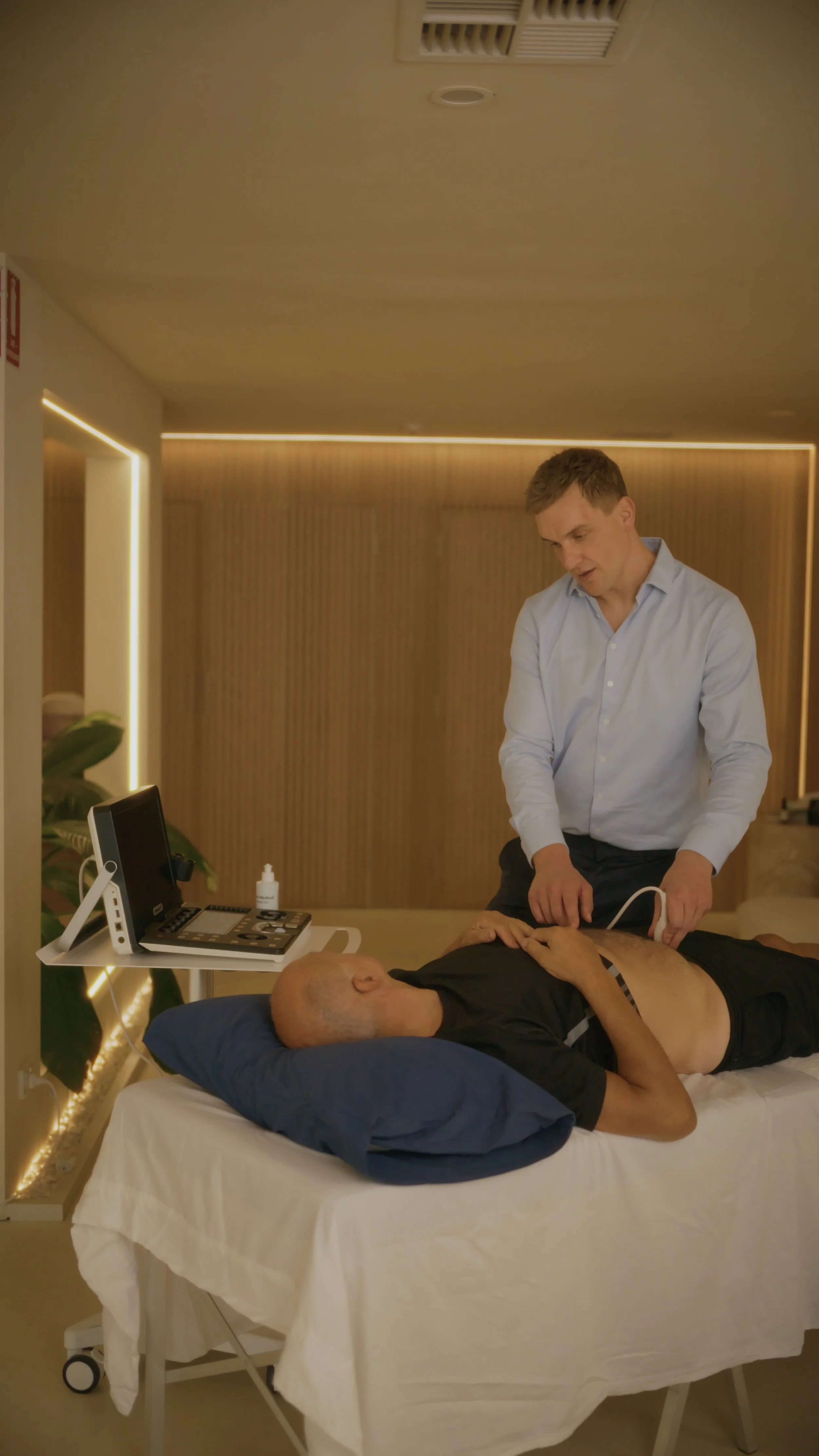
Normal Bowel Habits
Normal bowel motions can vary anywhere from 1 times per day to 3 times per week. You should be able to pass a stool that is soft, formed, without straining. You should be able to delay a bowel movement for a short time without urgency or leakage, only need to sit there for a short time and feel like you have fully emptied after your bowel motion. There should be no pain or bleeding.
Signs there may be an issue
Constipation, hard stools, or frequent straining
Urgency or difficulty holding on
Incomplete emptying or repeated trips to the toilet
Bowel leakage, having an accident, or soiled underwear after a bowel motion
Pain with bowel movements, bloating, or pelvic/anal discomfort
Symptoms following colorectal or pelvic surgery
Bowel Health Physiotherapy for Men - Sydney
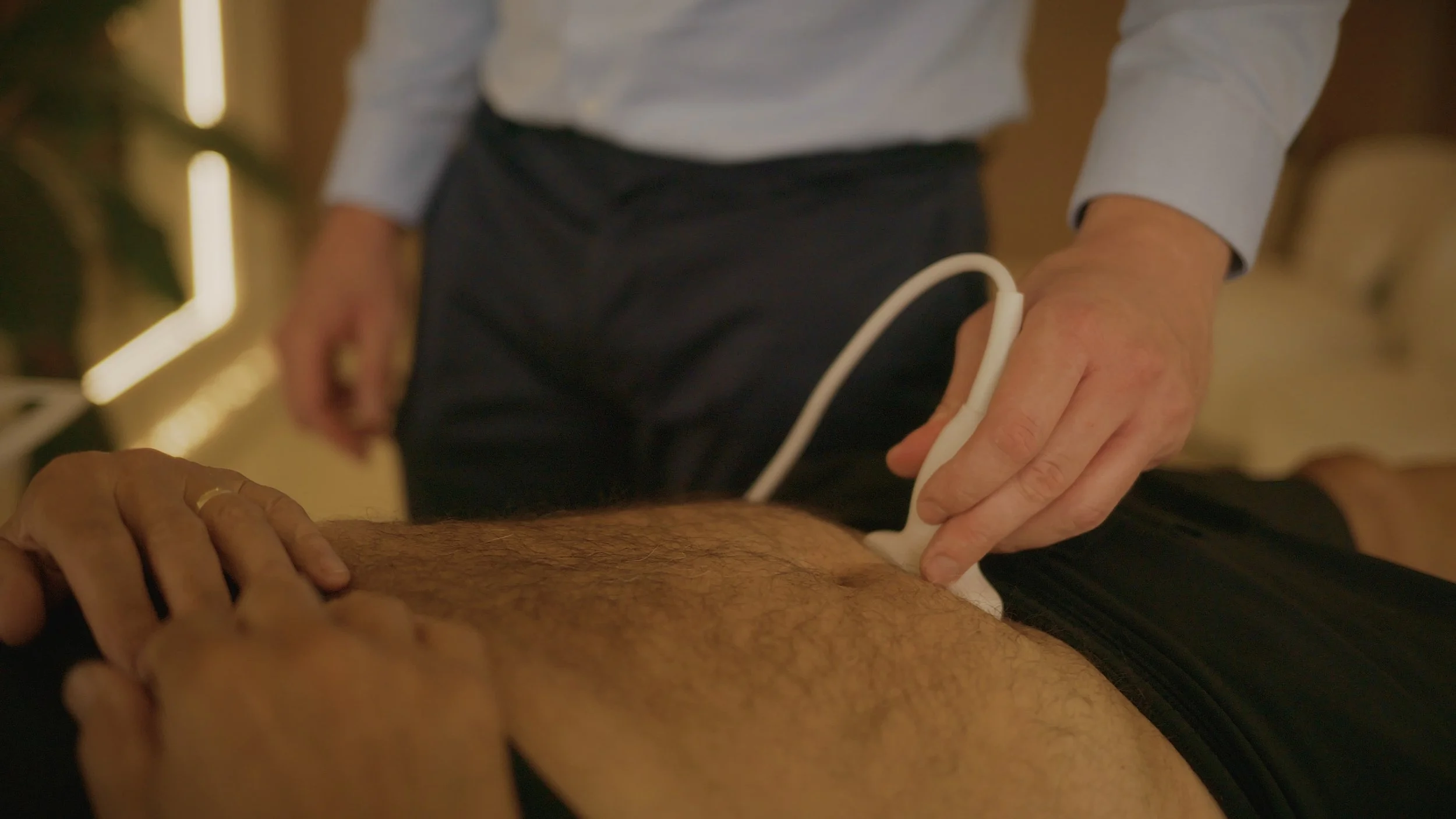
How Atlas Physiotherapy Can Help
Detailed assessment of bowel habits, diet, toileting posture, and pelvic floor function
Pelvic floor retraining (relaxation, coordination, or strengthening as needed)
Education on toileting mechanics, breathing, and pressure management
Strategies to improve stool consistency and bowel regularity (in collaboration with your GP or specialist)
Support with return to activity and long-term symptom management

Prostate Cancer Rehabilitation & Prostate Health Physiotherapy
At Atlas Physiotherapy, Sydney, we provide pre- and post-operative physiotherapy for men undergoing radical prostatectomy or other prostate treatments. Prehabilitation before surgery and structured rehabilitation afterwards significantly improve continence recovery and quality of life outcomes.
What Does the Prostate Do?
The prostate is a small gland, about the size of a walnut, that sits just below the bladder and surrounds part of the urethra (the tube that carries urine out of the body). It also has a role in reproduction - it produces fluid that mixes with sperm to create semen. This fluid helps nourish and protect sperm.
Because of its position around the urethra and just above the pelvic floor muscles, changes in prostate size or treatment involving the prostate can affect bladder control, sexual function, and pelvic comfort.

Signs and Symptoms of Prostate Enlargement (BPH)
Benign Prostatic Hyperplasia (BPH) is a non-cancerous enlargement of the prostate that becomes more common with age.
Common urinary symptoms:
Increased urinary frequency (especially at night)
Urgency - feeling a sudden need to rush to the toilet
Difficulty starting urination
Weak or slow urine stream
Dribbling at the end of urination
Feeling that the bladder hasn’t fully emptied
Straining to pass urine

Signs and Symptoms of Prostate Cancer
Early prostate cancer may not cause noticeable symptoms. When symptoms do occur, they can overlap with BPH.
Possible symptoms include:
Changes in urinary flow (weak stream, hesitancy)
Increased urinary frequency, particularly at night
Blood in urine or semen
Erectile dysfunction
Pain or discomfort in the pelvic area
Unexplained lower back, hip, or pelvic pain (in more advanced cases)
Unintended weight loss or fatigue (less common, later-stage signs)
Any persistent change in urinary or sexual function should be medically assessed.

How Physiotherapy Helps Before and After Radical Prostatectomy
A radical prostatectomy (surgical removal of the prostate) is a common treatment for prostate cancer. Because the prostate sits closely with the urinary sphincter and pelvic floor muscles, surgery can affect bladder control and sexual function.
Before Surgery (Prehabilitation)
Physiotherapy can:
Assess your baseline pelvic floor muscle strength and control
Teach correct pelvic floor muscle activation
Improve endurance and coordination of the urinary sphincter
Educate on bladder habits and post-operative expectations
Help men enter surgery stronger and more confident
Research shows that men who begin pelvic floor training before surgery often recover continence more quickly.

After Surgery
Physiotherapy can support recovery by:
Guiding structured pelvic floor rehabilitation
Improving bladder control and reducing leakage
Addressing urgency and frequency
Assisting with return to exercise and daily activities
Supporting erectile function recovery through targeted pelvic floor training
Managing pelvic pain or scar-related discomfort
earl
Recovery timelines vary, but early and guided rehabilitation significantly improves outcomes.

Physiotherapy for Erectile Dysfunction & Premature Ejaculation - Sydney
Many men are unaware that physiotherapy can play an important role in treating erectile dysfunction and premature ejaculation - particularly when the pelvic floor muscles are contributing. At Atlas Physiotherapy in Sydney, treatment is discreet, evidence-based, and individually tailored.
Erectile Dysfunction & Premature Ejaculation
Erectile dysfunction is the ongoing difficulty achieving or maintaining an erection firm enough for satisfying sexual activity. Premature ejaculation is when ejaculation occurs sooner than desired, often with minimal stimulation and limited voluntary control. It can be lifelong or develop later in life.
The pelvic floor muscles play a key role in both erection quality and ejaculatory control. They help maintain penile rigidity by supporting blood retention during erection and contribute to the timing and control of ejaculation. When these muscles are weak, poorly coordinated, or overly tense, sexual performance can be affected.
Difficulties with erections or ejaculation are common and treatable - and they’re far more physical than many men realise.

Signs and Symptoms
Erectile Dysfunction (ED)
Difficulty achieving an erection
Difficulty maintaining an erection
Erections that are less firm than previously
Reduced spontaneous or morning erections
Loss of confidence during intimacy
Urinary leakage during sexual activity (in some men)
Premature Ejaculation (PE)
Ejaculation sooner than desired
Limited ability to delay climax
Feeling of reduced control
Performance anxiety or avoidance of intimacy
Pelvic tension or discomfort
Fluctuating erection firmness
These conditions can overlap. For example, pelvic floor overactivity can contribute to both early ejaculation and unstable erections.

How Atlas Physiotherapy Can Help
Treatment is tailored to the individual and may involve strengthening, relaxation, or coordination retraining - depending on what assessment findings show.
Physiotherapy may include:
Assessment of pelvic floor strength, endurance, and tone
Identifying weakness versus overactivity
Targeted strengthening where muscle support is insufficient
Down-training and relaxation techniques for overly tense muscles
Retraining muscle timing and control
For many men, improving pelvic floor control significantly improves erectile firmness, ejaculatory control, and sexual confidence.

Peyronie's Disease Treatment
Peyronie’s disease is a condition where fibrous scar tissue (plaque) develops within the shaft of the penis. This can cause curvature, narrowing, shortening, or pain during erection.
It typically develops gradually and may be linked to minor repetitive trauma, genetic factors, or connective tissue changes. While the exact cause isn’t always clear, the condition is physical - not psychological.
After a radical prostatectomy there is a 1 in 6 chance of developing Peyronie’s disease, and connective tissue disorders like Dupuytren's disease also increases the likelihood of developing the disease.
Signs and Symptoms of Peyronie’s Disease
Visible penile curvature during erection
A palpable lump or firm plaque within the shaft
Pain, particularly during erection (more common early on)
Loss of length or narrowing (“hourglass” shape)
Erectile dysfunction
Difficulty with penetration
Reduced sexual confidence
If curvature develops or changes suddenly, medical assessment is important to confirm diagnosis and rule out other causes.
How Atlas Physiotherapy Can Help
Physiotherapy does not remove plaque, but it can play an important role in managing symptoms and improving function.
Treatment may include:
Therapeutic ultrasound treatment to reduce the size of the plaque
Assessment of erectile function and pelvic floor involvement
Addressing contributing pelvic floor tension
Improving erectile rigidity through targeted muscle training
Penile rehabilitation strategies (when appropriate)
Supporting overall pelvic health and confidence
In some cases, physiotherapy may complement medical treatments such as medication or traction therapy.
Early assessment can be helpful to optimise function and reduce secondary issues such as pelvic floor overactivity or performance anxiety.

Male Pelvic Pain Physiotherapy - Chronic Pelvic Pain Syndrome
Chronic pelvic pain in men is often misdiagnosed or undertreated. At Atlas Physiotherapy in Leichhardt, we take a thorough, whole-body approach to assessing and treating male pelvic pain - including conditions such as chronic pelvic pain syndrome (CPPS), non-bacterial prostatitis, and pudendal neuralgia.
Male pelvic pain can feel confusing and frustrating - particularly when scans and tests don’t show a clear cause. Pain in this region is often related to the pelvic floor muscles, surrounding nerves, or persistent muscle tension rather than infection or structural damage.
The pelvic floor muscles sit at the base of the pelvis and help control bladder, bowel, and sexual function. When these muscles become overactive, tense, or poorly coordinated, they can contribute to ongoing discomfort.
Pelvic pain may be diagnosed under terms such as:
Chronic pelvic pain syndrome (CPPS)
Prostatitis (non-bacterial)
Pudendal neuralgia

Signs and Symptoms of Male Pelvic Pain
Symptoms vary between individuals but may include:
Aching or burning pain in the perineum (between the scrotum and anus)
Testicular or penile pain
Pain at the tip of the penis
Lower abdominal or suprapubic discomfort
Tailbone pain
Pain with sitting
Pain after ejaculation
Urinary urgency or frequency, or difficult initiating urination
A sensation of pelvic tightness or pressure

How Atlas Physiotherapy Can Help
Pelvic pain is rarely a “strength” problem. More often, it involves overactivity, guarding, and nervous system sensitisation.
Physiotherapy focuses on calming and retraining the system.
Assessment may include:
Evaluating pelvic floor tone and tenderness
Assessing muscle coordination and relaxation capacity
Reviewing bladder, bowel, and sexual function
Identifying lifestyle or load-related triggers
Assessing breathing patterns and abdominal pressure control
Treatment may involve:
Down-training and relaxation techniques
Manual therapy where appropriate
Breathing retraining
Nervous system regulation strategies
Gradual return to activity and exercise
Education to reduce fear and improve confidence
Recovery is often gradual, but structured rehabilitation can significantly reduce pain and restore function.

Get In Touch
Book a Men's Health Physiotherapy Appointment in Sydney
If you're ready to book, use the link below. If you'd prefer to ask a question first, or you're not sure whether physiotherapy is right for your situation, feel free to get in touch - we're happy to help you figure out the best path forward.
Atlas Physiotherapy is located in Leichhardt, easily accessible from across Sydney's Inner West, including Annandale, Balmain, Petersham, Stanmore, Newtown, and Glebe.
If you’d like to ask a question, or if you’re unsure which service is right for you, feel free to reach out.
